What Is the Heart Rate for a Baby at 7 Weeks and 6 Days
Heart rate is the speed of the heartbeat measured by the number of contractions (beats) of the heart per minute (bpm). The heart rate can vary co-ordinate to the body's concrete needs, including the need to absorb oxygen and excrete carbon dioxide, but is besides modulated by numerous factors, including, only not limited to, genetics, concrete fitness, stress or psychological status, diet, drugs, hormonal status, surroundings, and illness/illness likewise every bit the interaction between and among these factors.[1] It is usually equal or shut to the pulse measured at whatever peripheral point.
The American Centre Clan states the normal resting adult human heart rate is 60–100 bpm.[ii] Tachycardia is a high heart charge per unit, defined as in a higher place 100 bpm at rest.[iii] Bradycardia is a low heart rate, divers as beneath 60 bpm at residue. When a human being sleeps, a heartbeat with rates around forty–50 bpm is mutual and is considered normal. When the heart is not beating in a regular design, this is referred to as an arrhythmia. Abnormalities of heart rate sometimes indicate illness.[4]
Physiology [edit]

While heart rhythm is regulated entirely by the sinoatrial node nether normal conditions, eye rate is regulated by sympathetic and parasympathetic input to the sinoatrial node. The accelerans nerve provides sympathetic input to the eye by releasing norepinephrine onto the cells of the sinoatrial node (SA node), and the vagus nerve provides parasympathetic input to the center by releasing acetylcholine onto sinoatrial node cells. Therefore, stimulation of the accelerans nerve increases heart rate, while stimulation of the vagus nervus decreases it.[5]
As water and blood are incompressible fluids, one of the physiological means to deliver more than blood to an organ is to increase heart rate.[4] Normal resting heart rates range from 60 to 100 bpm.[vi] [seven] [eight] [nine] Bradycardia is defined as a resting centre rate below sixty bpm. However, center rates from 50 to 60 bpm are mutual among salubrious people and practice not necessarily require special attention.[two] Tachycardia is divers as a resting centre charge per unit to a higher place 100 bpm, though persistent rest rates betwixt lxxx and 100 bpm, mainly if they are nowadays during slumber, may be signs of hyperthyroidism or anemia (run into beneath).[4]
- Fundamental nervous system stimulants such as substituted amphetamines increase heart rate.
- Cardinal nervous organisation depressants or sedatives decrease the middle charge per unit (apart from some particularly foreign ones with equally strange effects, such as ketamine which tin cause – amongst many other things – stimulant-like effects such as tachycardia).
There are many means in which the heart rate speeds up or slows down. Most involve stimulant-like endorphins and hormones being released in the brain, some of which are those that are 'forced'/'enticed' out by the ingestion and processing of drugs such as cocaine or atropine.[10] [xi] [12]
This section discusses target middle rates for salubrious persons, which would be inappropriately high for most persons with coronary artery disease.[thirteen]
Influences from the central nervous system [edit]
Cardiovascular centres [edit]
The heart rate is rhythmically generated by the sinoatrial node. It is also influenced by central factors through sympathetic and parasympathetic nerves.[14] Nervous influence over the heart rate is centralized within the two paired cardiovascular centres of the medulla oblongata. The cardioaccelerator regions stimulate activity via sympathetic stimulation of the cardioaccelerator nerves, and the cardioinhibitory centers subtract heart activeness via parasympathetic stimulation every bit ane component of the vagus nerve. During residual, both centers provide slight stimulation to the heart, contributing to autonomic tone. This is a similar concept to tone in skeletal muscles. Usually, vagal stimulation predominates every bit, left unregulated, the SA node would initiate a sinus rhythm of approximately 100 bpm.[xv]
Both sympathetic and parasympathetic stimuli menstruum through the paired cardiac plexus nearly the base of operations of the center. The cardioaccelerator center also sends additional fibers, forming the cardiac fretfulness via sympathetic ganglia (the cervical ganglia plus superior thoracic ganglia T1–T4) to both the SA and AV nodes, plus additional fibers to the atria and ventricles. The ventricles are more than richly innervated past sympathetic fibers than parasympathetic fibers. Sympathetic stimulation causes the release of the neurotransmitter norepinephrine (also known equally noradrenaline) at the neuromuscular junction of the cardiac nerves. This shortens the repolarization period, thus speeding the rate of depolarization and contraction, which results in an increased heartrate. It opens chemic or ligand-gated sodium and calcium ion channels, assuasive an influx of positively charged ions.[15]
Norepinephrine binds to the beta–one receptor. High claret pressure medications are used to block these receptors and so reduce the heart rate.[15]

Autonomic Innervation of the Centre – Cardioaccelerator and cardioinhibitory areas are components of the paired cardiac centers located in the medulla oblongata of the brain. They innervate the heart via sympathetic cardiac fretfulness that increase cardiac activity and vagus (parasympathetic) nerves that slow cardiac activity.[15]
Parasympathetic stimulation originates from the cardioinhibitory region of the brain[xvi] with impulses traveling via the vagus nervus (cranial nerve 10). The vagus nervus sends branches to both the SA and AV nodes, and to portions of both the atria and ventricles. Parasympathetic stimulation releases the neurotransmitter acetylcholine (ACh) at the neuromuscular junction. ACh slows HR by opening chemic- or ligand-gated potassium ion channels to deadening the rate of spontaneous depolarization, which extends repolarization and increases the time before the next spontaneous depolarization occurs. Without any nervous stimulation, the SA node would establish a sinus rhythm of approximately 100 bpm. Since resting rates are considerably less than this, it becomes evident that parasympathetic stimulation commonly slows HR. This is like to an individual driving a car with i foot on the brake pedal. To speed up, one need merely remove one's foot from the brake and permit the engine increase speed. In the case of the centre, decreasing parasympathetic stimulation decreases the release of ACh, which allows HR to increase upwardly to approximately 100 bpm. Whatsoever increases beyond this rate would require sympathetic stimulation.[fifteen]
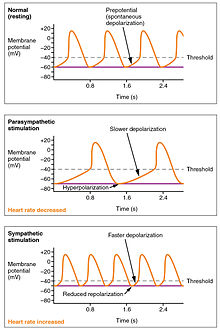
Furnishings of Parasympathetic and Sympathetic Stimulation on Normal Sinus Rhythm – The wave of depolarization in a normal sinus rhythm shows a stable resting Hour. Following parasympathetic stimulation, Hr slows. Following sympathetic stimulation, HR increases.[15]
Input to the cardiovascular centres [edit]
The cardiovascular centres receive input from a series of visceral receptors with impulses traveling through visceral sensory fibers within the vagus and sympathetic nerves via the cardiac plexus. Among these receptors are various proprioreceptors, baroreceptors, and chemoreceptors, plus stimuli from the limbic organization which normally enable the precise regulation of heart office, via cardiac reflexes. Increased physical activeness results in increased rates of firing by diverse proprioreceptors located in muscles, joint capsules, and tendons. The cardiovascular centres monitor these increased rates of firing, suppressing parasympathetic stimulation or increasing sympathetic stimulation equally needed in order to increase blood flow.[15]
Similarly, baroreceptors are stretch receptors located in the aortic sinus, carotid bodies, the venae cavae, and other locations, including pulmonary vessels and the right side of the middle itself. Rates of firing from the baroreceptors represent blood pressure level, level of physical action, and the relative distribution of claret. The cardiac centers monitor baroreceptor firing to maintain cardiac homeostasis, a mechanism chosen the baroreceptor reflex. With increased force per unit area and stretch, the rate of baroreceptor firing increases, and the cardiac centers subtract sympathetic stimulation and increase parasympathetic stimulation. As pressure and stretch decrease, the rate of baroreceptor firing decreases, and the cardiac centers increase sympathetic stimulation and decrease parasympathetic stimulation.[15]
At that place is a similar reflex, called the atrial reflex or Bainbridge reflex, associated with varying rates of blood menstruum to the atria. Increased venous render stretches the walls of the atria where specialized baroreceptors are located. Notwithstanding, as the atrial baroreceptors increase their rate of firing and as they stretch due to the increased blood pressure, the cardiac middle responds by increasing sympathetic stimulation and inhibiting parasympathetic stimulation to increase HR. The contrary is also truthful.[xv]
Increased metabolic byproducts associated with increased activity, such as carbon dioxide, hydrogen ions, and lactic acid, plus falling oxygen levels, are detected past a suite of chemoreceptors innervated past the glossopharyngeal and vagus nerves. These chemoreceptors provide feedback to the cardiovascular centers about the need for increased or decreased claret menses, based on the relative levels of these substances.[15]
The limbic arrangement can also significantly touch HR related to emotional state. During periods of stress, information technology is not unusual to place college than normal HRs, ofttimes accompanied by a surge in the stress hormone cortisol. Individuals experiencing extreme feet may manifest panic attacks with symptoms that resemble those of middle attacks. These events are typically transient and treatable. Meditation techniques accept been developed to ease anxiety and have been shown to lower HR effectively. Doing simple deep and slow breathing exercises with one's eyes closed can also significantly reduce this anxiety and HR.[15]
Factors influencing heart rate [edit]
| ||||||||||||||||||||||||||
|
Using a combination of autorhythmicity and innervation, the cardiovascular center is able to provide relatively precise control over the heart rate, but other factors tin can impact on this. These include hormones, notably epinephrine, norepinephrine, and thyroid hormones; levels of various ions including calcium, potassium, and sodium; body temperature; hypoxia; and pH balance.[fifteen]
Epinephrine and norepinephrine [edit]
The catecholamines, epinephrine and norepinephrine, secreted by the adrenal medulla course i component of the extended fight-or-flying machinery. The other component is sympathetic stimulation. Epinephrine and norepinephrine take similar effects: binding to the beta-1 adrenergic receptors, and opening sodium and calcium ion chemical- or ligand-gated channels. The rate of depolarization is increased past this additional influx of positively charged ions, so the threshold is reached more than apace and the period of repolarization is shortened. Nevertheless, massive releases of these hormones coupled with sympathetic stimulation may actually pb to arrhythmias. In that location is no parasympathetic stimulation to the adrenal medulla.[fifteen]
Thyroid hormones [edit]
In general, increased levels of the thyroid hormones (thyroxine(T4) and triiodothyronine (T3)), increment the heart rate; excessive levels tin can trigger tachycardia. The impact of thyroid hormones is typically of a much longer duration than that of the catecholamines. The physiologically active form of triiodothyronine, has been shown to directly enter cardiomyocytes and change activity at the level of the genome.[ clarification needed ] It also impacts the beta adrenergic response like to epinephrine and norepinephrine.[15]
Calcium [edit]
Calcium ion levels take a dandy impact on center rate and contractility: increased calcium levels cause an increase in both. Loftier levels of calcium ions outcome in hypercalcemia and excessive levels tin induce cardiac arrest. Drugs known every bit calcium channel blockers wearisome Hr past binding to these channels and blocking or slowing the inward movement of calcium ions.[fifteen]
Caffeine and nicotine [edit]
Caffeine and nicotine are both stimulants of the nervous system and of the cardiac centres causing an increased heart rate. Caffeine works past increasing the rates of depolarization at the SA node, whereas nicotine stimulates the action of the sympathetic neurons that deliver impulses to the middle.[xv] Both stimulants are legal and unregulated, and nicotine is very addictive.[15]
Effects of stress [edit]
Both surprise and stress induce physiological response: elevate heart charge per unit substantially.[17] In a report conducted on 8 female and male student actors ages 18 to 25, their reaction to an unforeseen occurrence (the cause of stress) during a performance was observed in terms of heart charge per unit. In the data collected, there was a noticeable trend between the location of actors (onstage and offstage) and their elevation in heart charge per unit in response to stress; the actors nowadays offstage reacted to the stressor immediately, demonstrated by their immediate peak in middle charge per unit the minute the unexpected event occurred, simply the actors nowadays onstage at the time of the stressor reacted in the following 5 minute menses (demonstrated by their increasingly elevated heart rate). This trend regarding stress and heart rate is supported by previous studies; negative emotion/stimulus has a prolonged outcome on heart rate in individuals who are directly impacted.[18] In regard to the characters present onstage, a reduced startle response has been associated with a passive defense, and the diminished initial middle charge per unit response has been predicted to have a greater tendency to dissociation.[19] Current evidence suggests that heart charge per unit variability can be used as an accurate mensurate of psychological stress and may be used for an objective measurement of psychological stress.[20]
Factors decreasing heart rate [edit]
The heart charge per unit can be slowed by contradistinct sodium and potassium levels, hypoxia, acidosis, alkalosis, and hypothermia. The relationship between electrolytes and HR is complex, simply maintaining electrolyte residuum is critical to the normal moving ridge of depolarization. Of the two ions, potassium has the greater clinical significance. Initially, both hyponatremia (depression sodium levels) and hypernatremia (high sodium levels) may atomic number 82 to tachycardia. Severely high hypernatremia may lead to fibrillation, which may cause CO to terminate. Severe hyponatremia leads to both bradycardia and other arrhythmias. Hypokalemia (low potassium levels) also leads to arrhythmias, whereas hyperkalemia (loftier potassium levels) causes the heart to go weak and flaccid, and ultimately to fail.[15]
Heart muscle relies exclusively on aerobic metabolism for energy. Severe myocardial infarction (commonly called a center assault) can lead to a decreasing heart rate, since metabolic reactions fueling eye contraction are restricted.[xv]
Acidosis is a status in which excess hydrogen ions are present, and the patient's blood expresses a low pH value. Alkalosis is a condition in which there are too few hydrogen ions, and the patient's blood has an elevated pH. Normal blood pH falls in the range of 7.35–7.45, so a number lower than this range represents acidosis and a higher number represents alkalosis. Enzymes, being the regulators or catalysts of virtually all biochemical reactions – are sensitive to pH and will change shape slightly with values outside their normal range. These variations in pH and accompanying slight physical changes to the agile site on the enzyme subtract the rate of formation of the enzyme-substrate complex, afterwards decreasing the rate of many enzymatic reactions, which tin have complex effects on HR. Severe changes in pH will lead to denaturation of the enzyme.[15]
The concluding variable is body temperature. Elevated body temperature is called hyperthermia, and suppressed body temperature is chosen hypothermia. Slight hyperthermia results in increasing HR and strength of contraction. Hypothermia slows the rate and strength of centre contractions. This distinct slowing of the middle is one component of the larger diving reflex that diverts blood to essential organs while submerged. If sufficiently chilled, the heart will stop chirapsia, a technique that may be employed during open centre surgery. In this example, the patient's claret is usually diverted to an artificial center-lung auto to maintain the body's blood supply and gas commutation until the surgery is complete, and sinus rhythm can be restored. Excessive hyperthermia and hypothermia volition both result in death, as enzymes bulldoze the body systems to stop normal function, kickoff with the key nervous organisation.[15]
Physiological control over heart rate [edit]


A report shows that bottlenose dolphins can acquire – apparently via instrumental workout – to quickly and selectively tiresome downward their heart charge per unit during diving for conserving oxygen depending on external signals. In humans regulating heart charge per unit by methods such equally listening to music, meditation or a vagal maneuver takes longer and only lowers the charge per unit to a much smaller extent.[21]
In different circumstances [edit]

Eye rate (60 minutes) (top trace) and tidal book (Vt) (lung volume, second trace) plotted on the aforementioned nautical chart, showing how heart rate increases with inspiration and decreases with expiration.
Heart rate is not a stable value and it increases or decreases in response to the body'southward demand in a way to maintain an equilibrium (basal metabolic rate) between requirement and delivery of oxygen and nutrients. The normal SA node firing rate is affected by autonomic nervous system action: sympathetic stimulation increases and parasympathetic stimulation decreases the firing rate.[22] A number of dissimilar metrics are used to depict center rate.[ citation needed ]
Resting center rate [edit]
Normal pulse rates at rest, in beats per infinitesimal (BPM):[23]
| newborn (0–1 months old) | infants (one – 11 months) | children (ane – 2 years one-time) | children (three – 4 years) | children (five – 6 years) | children (seven – ix years) | children over ten years & adults, including seniors | well-trained adult athletes |
|---|---|---|---|---|---|---|---|
| 70-190 | 80–160 | 80-130 | 80-120 | 75–115 | 70–110 | 60–100 | 40–60 |
The basal or resting middle rate (Hrbalance) is defined as the heart charge per unit when a person is awake, in a neutrally temperate environs, and has not been subject to any recent exertion or stimulation, such every bit stress or surprise. The available evidence indicates that the normal range for resting middle charge per unit is 50-90 beats per minute.[6] [seven] [8] [9] This resting center rate is often correlated with bloodshed. For example, all-crusade mortality is increased by 1.22 (take chances ratio) when heart charge per unit exceeds 90 beats per minute.[6] The mortality rate of patients with myocardial infarction increased from fifteen% to 41% if their access heart rate was greater than xc beats per minute.[vii] ECG of 46,129 individuals with low risk for cardiovascular disease revealed that 96% had resting heart rates ranging from 48 to 98 beats per infinitesimal.[8] Finally, in i study 98% of cardiologists suggested that as a desirable target range, 50 to 90 beats per minute is more appropriate than 60 to 100.[9] The normal resting heart rate is based on the at-rest firing rate of the heart's sinoatrial node, where the faster pacemaker cells driving the self-generated rhythmic firing and responsible for the heart's autorhythmicity are located.[24] For endurance athletes at the elite level, information technology is not unusual to have a resting middle rate betwixt 33 and 50 bpm.[ citation needed ]
Maximum centre rate [edit]
The maximum heart charge per unit (HRmax) is the highest heart charge per unit an individual can achieve without astringent bug through do stress,[25] [ unreliable medical source? ] [26] and generally decreases with age. Since HRmax varies by individual, the most accurate way of measuring any single person's HRmax is via a cardiac stress test. In this test, a person is subjected to controlled physiologic stress (more often than not past treadmill) while being monitored by an ECG. The intensity of exercise is periodically increased until certain changes in heart office are detected on the ECG monitor, at which betoken the bailiwick is directed to finish. Typical duration of the test ranges ten to twenty minutes.[ citation needed ]
The theoretical maximum heart rate of a human being is 300bpm, yet there accept been multiple cases where this theoretical upper limit has been exceeded. The fastest homo ventricular conduction rate recorded to this day is a conducted tachyarrhythmia with ventricular rate of 480 beats per minute,[27] which is comparable to the heart rate of a mouse.
Adults who are beginning a new exercise regimen are frequently brash to perform this test only in the presence of medical staff due to risks associated with loftier heart rates. For full general purposes, a formula is often employed to estimate a person's maximum center rate. However, these predictive formulas have been criticized as inaccurate because they generalized population-averages and usually focus on a person's age and practice non even have normal resting pulse rate into consideration. It is well-established that at that place is a "poor relationship between maximal heart charge per unit and age" and large standard deviations relative to predicted center rates.[28] (see Limitations of Interpretation Formulas).

The various formulae provide slightly different numbers for the maximum center rates past age.
A number of formulas are used to estimate HRmax
Nes, et al. (2013) [edit]
Based on measurements of 3320 salubrious men and women anile between xix and 89, and including the potential modifying effect of gender, body composition, and physical activity, Nes et al establish:
- 60 minutesmax = 211 − (0.64 × age)[29]
This relationship was found to concur the essentially regardless of gender, concrete activity condition, maximal oxygen uptake, smoking, or trunk mass index. However, a standard error of the approximate of 10.viii beats/min must be accounted for when applying the formula to clinical settings, and the researchers concluded that actual measurement via a maximal test may be preferable whenever possible.[29]
Tanaka, Monahan, & Seals [edit]
From Tanaka, Monahan, & Seals (2001):
- HRmax = 208 − (0.7 × age)[30]
Their meta-analysis (of 351 prior studies involving 492 groups and 18,712 subjects) and laboratory study (of 514 healthy subjects) concluded that, using this equation, HRmax was very strongly correlated to age (r = −0.90). The regression equation that was obtained in the laboratory-based written report (209 − 0.7 ten age), was virtually identical to that of the meta-study. The results showed HRmax to be contained of gender and independent of wide variations in habitual physical activity levels. This study plant a standard divergence of ~10 beats per minute for individuals of any age, meaning the HRmax formula given has an accuracy of ±20 beats per minute.[xxx]
Oakland University [edit]
In 2007, researchers at the Oakland University analyzed maximum heart rates of 132 individuals recorded yearly over 25 years, and produced a linear equation very similar to the Tanaka formula, HRmax = 207 − (0.7 × historic period), and a nonlinear equation, 60 minutesmax = 192 − (0.007 × age2). The linear equation had a conviction interval of ±five–8 bpm and the nonlinear equation had a tighter range of ±2–five bpm[31]
Haskell & Fox [edit]

Fox and Haskell formula; widely used.
Notwithstanding the research of Tanaka, Monahan, & Seals, the well-nigh widely cited formula for Hourmax (which contains no reference to any standard deviation) is still:[32]
- HRmax = 220 − age
Although attributed to various sources, information technology is widely thought to have been devised in 1970 past Dr. William Haskell and Dr. Samuel Fox.[33] Research into the history of this formula reveals that information technology was non adult from original enquiry, but resulted from ascertainment based on information from approximately 11 references consisting of published enquiry or unpublished scientific compilations.[34] It gained widespread use through beingness used by Polar Electro in its heart rate monitors,[33] which Dr. Haskell has "laughed well-nigh",[33] as the formula "was never supposed to be an absolute guide to rule people's training."[33]
While it is the most mutual (and easy to call up and calculate), this item formula is not considered past reputable health and fitness professionals to be a good predictor of HRmax. Despite the widespread publication of this formula, enquiry spanning two decades reveals its big inherent error, Sxy = seven–11 bpm. Consequently, the estimation calculated past 60 minutesmax = 220 − age has neither the accuracy nor the scientific merit for use in exercise physiology and related fields.[34]
Robergs & Landwehr [edit]
A 2002 report[34] of 43 dissimilar formulas for HRmax (including that of Haskell and Fox – come across in a higher place) published in the Journal of Exercise Psychology concluded that:[ citation needed ]
- no "acceptable" formula currently existed (they used the term "adequate" to hateful acceptable for both prediction of VO2, and prescription of exercise grooming HR ranges)
- the least objectionable formula (Inbar, et al., 1994) was:
-
- 60 minutesmax = 205.8 − (0.685 × age) [35]
- This had a standard divergence that, although large (6.4 bpm), was considered acceptable for prescribing exercise training HR ranges.[ citation needed ]
Gulati (for women) [edit]
Inquiry conducted at Northwestern University by Martha Gulati, et al., in 2010[36] suggested a maximum center charge per unit formula for women:
- Hrmax = 206 − (0.88 × age)
Wohlfart, B. and Farazdaghi, G.R. [edit]
A 2003 study from Lund, Sweden gives reference values (obtained during bike ergometry) for men:
- Hrmax = 203.7 / ( 1 + exp( 0.033 × (age − 104.3) ) )[37]
and for women:
- Hourmax = 190.two / ( i + exp( 0.0453 × (age − 107.5) ) )[38]
Limitations [edit]
Maximum heart rates vary significantly between individuals.[33] Even within a single elite sports squad, such every bit Olympic rowers in their 20s, maximum heart rates have been reported every bit varying from 160 to 220.[33] Such a variation would equate to a sixty or 90 year age gap in the linear equations above, and would seem to point the extreme variation about these average figures.[ commendation needed ]
Figures are more often than not considered averages, and depend greatly on private physiology and fettle. For example, an endurance runner's rates will typically exist lower due to the increased size of the eye required to support the practice, while a sprinter'southward rates will be higher due to the improved response fourth dimension and short duration. While each may have predicted heart rates of 180 (= 220 − historic period), these two people could take actual Hourmax 20 beats apart (e.thousand., 170–190).[ commendation needed ]
Further, note that individuals of the same age, the aforementioned grooming, in the aforementioned sport, on the same team, can have actual Hourmax 60 bpm autonomously (160–220):[33] the range is extremely wide, and some say "The eye rate is probably the least important variable in comparing athletes."[33]
Heart rate reserve [edit]
Heart rate reserve (60 minutesreserve) is the difference betwixt a person'south measured or predicted maximum heart rate and resting heart rate. Some methods of measurement of practice intensity measure percent of centre charge per unit reserve. Additionally, every bit a person increases their cardiovascular fitness, their Hourrest will drop, and the heart rate reserve will increase. Percentage of Hourreserve is equivalent to percent of VOtwo reserve.[39]
- Hrreserve = HRmax − HRremainder
This is often used to gauge practise intensity (showtime used in 1957 past Karvonen).[40]
Karvonen's report findings accept been questioned, due to the following:
- The study did not utilise VO2 data to develop the equation.
- Only six subjects were used, and the correlation between the percentages of HRreserve and VOii max was not statistically significant.[41]
Target heart rate [edit]
For salubrious people, the Target Heart Rate (THR) or Grooming Heart Rate Range (THRR) is a desired range of centre rate reached during aerobic practise which enables one's eye and lungs to receive the most benefit from a workout. This theoretical range varies based generally on age; however, a person'south physical condition, sex, and previous training also are used in the calculation. Below are ii ways to calculate i'south THR. In each of these methods, there is an element chosen "intensity" which is expressed as a percentage. The THR can exist calculated as a range of 65–85% intensity. Even so, it is crucial to derive an accurate HRmax to ensure these calculations are meaningful.[ commendation needed ]
Example for someone with a HRmax of 180 (age 40, estimating 60 minutesmax As 220 − age):
- 65% Intensity: (220 − (historic period = twoscore)) × 0.65 → 117 bpm
- 85% Intensity: (220 − (age = xl)) × 0.85 → 154bpm
Karvonen method [edit]
The Karvonen method factors in resting heart rate (60 minutesresiduum) to calculate target middle charge per unit (THR), using a range of l–85% intensity:[42]
- THR = ((HRmax − HRrest) × % intensity) + Hourrest
Equivalently,
- THR = (Hourreserve × % intensity) + Hrrest
Case for someone with a HRmax of 180 and a Hrresiduum of 70 (and therefore a Hrreserve of 110):
- 50% Intensity: ((180 − 70) × 0.50) + seventy = 125 bpm
- 85% Intensity: ((180 − 70) × 0.85) + 70 = 163 bpm
Zoladz method [edit]
An alternative to the Karvonen method is the Zoladz method, which is used to test an athlete's capabilities at specific heart rates. These are not intended to exist used equally exercise zones, although they are oftentimes used as such.[43] The Zoladz test zones are derived by subtracting values from HRmax:
- THR = HRmax − Adjuster ± 5 bpm
- Zone ane Adjuster = l bpm
- Zone 2 Adjuster = twoscore bpm
- Zone 3 Adjuster = xxx bpm
- Zone 4 Adjuster = 20 bpm
- Zone 5 Adjuster = 10 bpm
Case for someone with a HRmax of 180:
- Zone ane(easy exercise): 180 − 50 ± v → 125 − 135 bpm
- Zone iv(tough exercise): 180 − 20 ± 5 → 155 − 165 bpm
Heart rate recovery [edit]
Centre charge per unit recovery (HRR) is the reduction in heart rate at peak exercise and the rate as measured after a cool-down flow of fixed elapsing.[44] A greater reduction in heart charge per unit after exercise during the reference menses is associated with a college level of cardiac fettle.[45]
Heart rates that practice not drop by more than 12 bpm one minute after stopping exercise are associated with an increased adventure of death.[44] People with an abnormal HRR divers as a subtract of 42 beats per minutes or less at two minutes post-exercise had a mortality charge per unit 2.5 times greater than patients with a normal recovery.[45] Another study reported a four-fold increase in mortality in subjects with an abnormal HRR defined as ≤12 bpm reduction one minute subsequently the cessation of do.[45] A study reported that a HRR of ≤22 bpm after two minutes "best identified loftier-run a risk patients".[45] They also found that while HRR had meaning prognostic value it had no diagnostic value.[45] [46]
Development [edit]
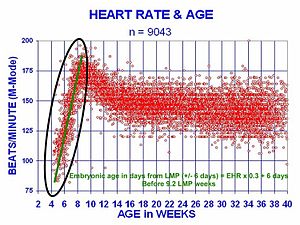
At 21 days later conception, the human heart begins beating at seventy to lxxx beats per minute and accelerates linearly for the first month of beating.
The human heart beats more than than 2.viii billion times in an boilerplate lifetime.[47]
The heartbeat of a human being embryo begins at approximately 21 days after conception, or five weeks later on the terminal normal menstrual period (LMP), which is the appointment normally used to date pregnancy in the medical community. The electrical depolarizations that trigger cardiac myocytes to contract arise spontaneously within the myocyte itself. The heartbeat is initiated in the pacemaker regions and spreads to the residuum of the heart through a conduction pathway. Pacemaker cells develop in the primitive atrium and the sinus venosus to form the sinoatrial node and the atrioventricular node respectively. Conductive cells develop the packet of His and acquit the depolarization into the lower eye.[ citation needed ]
The human heart begins chirapsia at a rate near the mother's, nigh 75–80 beats per minute (bpm). The embryonic eye charge per unit and then accelerates linearly for the outset calendar month of beating, peaking at 165–185 bpm during the early 7th week, (early ninth week subsequently the LMP). This acceleration is approximately three.3 bpm per mean solar day, or about x bpm every three days, an increase of 100 bpm in the beginning month.[48]
After peaking at almost 9.2 weeks after the LMP, it decelerates to near 150 bpm (+/-25 bpm) during the 15th week subsequently the LMP. After the 15th week the deceleration slows reaching an average rate of about 145 (+/-25 bpm) bpm at term. The regression formula which describes this dispatch before the embryo reaches 25 mm in crown-rump length or 9.ii LMP weeks is:
Clinical significance [edit]
Transmission measurement [edit]


Heart charge per unit monitor with a wrist receiver
Heart rate is measured by finding the pulse of the heart. This pulse rate can be found at any betoken on the trunk where the artery'south pulsation is transmitted to the surface by pressuring information technology with the index and middle fingers; often it is compressed against an underlying structure like bone. The thumb should non exist used for measuring another person's eye rate, as its strong pulse may interfere with the right perception of the target pulse.[ citation needed ]
The radial artery is the easiest to use to bank check the middle rate. Withal, in emergency situations the most reliable arteries to measure center rate are carotid arteries. This is important mainly in patients with atrial fibrillation, in whom centre beats are irregular and stroke book is largely different from one beat to another. In those beats post-obit a shorter diastolic interval left ventricle does non fill properly, stroke book is lower and pulse moving ridge is not potent plenty to be detected by palpation on a distal avenue like the radial artery. Information technology tin be detected, however, past doppler.[49] [fifty]
Possible points for measuring the middle rate are:[ commendation needed ]
- The ventral attribute of the wrist on the side of the thumb (radial artery).
- The ulnar artery.
- The inside of the elbow, or under the biceps musculus (brachial artery).
- The groin (femoral artery).
- Behind the medial malleolus on the feet (posterior tibial avenue).
- Middle of dorsum of the foot (dorsalis pedis).
- Behind the knee (popliteal artery).
- Over the abdomen (abdominal aorta).
- The chest (noon of the heart), which can be felt with i's hand or fingers. It is as well possible to auscultate the heart using a stethoscope.
- In the neck, lateral of the larynx (carotid artery)
- The temple (superficial temporal avenue).
- The lateral edge of the mandible (facial artery).
- The side of the head virtually the ear (posterior auricular avenue).

Electronic measurement [edit]

In obstetrics, heart rate can be measured past ultrasonography, such every bit in this embryo (at lesser left in the sac) of 6 weeks with a heart rate of approximately 90 per minute.
A more than precise method of determining heart rate involves the use of an electrocardiograph, or ECG (also abbreviated EKG). An ECG generates a pattern based on electrical activity of the centre, which closely follows centre function. Continuous ECG monitoring is routinely washed in many clinical settings, especially in critical care medicine. On the ECG, instantaneous heart rate is calculated using the R wave-to-R moving ridge (RR) interval and multiplying/dividing in order to derive middle rate in heartbeats/min. Multiple methods exist:[ citation needed ]
- HR = one thousand*60/(RR interval in milliseconds)
- HR = lx/(RR interval in seconds)
- Hr = 300/number of "large" squares between successive R waves.
- Hour= 1,500 number of big blocks
Center rate monitors allow measurements to be taken continuously and tin be used during practise when manual measurement would be difficult or impossible (such equally when the easily are existence used). Various commercial middle rate monitors are also available. Some monitors, used during sport, consist of a chest strap with electrodes. The bespeak is transmitted to a wrist receiver for display.[ citation needed ]
Alternative methods of measurement include seismocardiography.[51]
Optical measurements [edit]
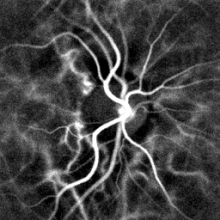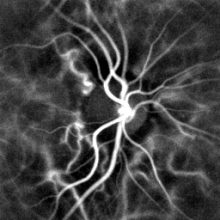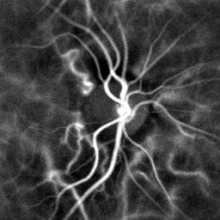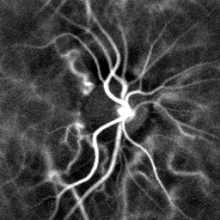
Pulse oximetry of the finger and laser Doppler imaging of the eye fundus are oft used in the clinics. Those techniques can appraise the heart rate by measuring the delay between pulses.[ commendation needed ]
Tachycardia [edit]
Tachycardia is a resting heart charge per unit more than than 100 beats per infinitesimal. This number can vary as smaller people and children take faster center rates than average adults.
Physiological conditions where tachycardia occurs:
- Pregnancy
- Emotional weather condition such as anxiety or stress.
- Practise
Pathological conditions where tachycardia occurs:
- Sepsis
- Fever
- Anemia
- Hypoxia
- Hyperthyroidism
- Hypersecretion of catecholamines
- Cardiomyopathy
- Valvular heart diseases
- Astute Radiation Syndrome
Bradycardia [edit]
Bradycardia was defined as a centre rate less than 60 beats per minute when textbooks asserted that the normal range for eye rates was threescore–100 bpm. The normal range has since been revised in textbooks to 50–ninety bpm for a human being at total rest. Setting a lower threshold for bradycardia prevents misclassification of fit individuals as having a pathologic center rate. The normal middle rate number can vary equally children and adolescents tend to accept faster heart rates than average adults. Bradycardia may be associated with medical conditions such as hypothyroidism.[53]
Trained athletes tend to have slow resting heart rates, and resting bradycardia in athletes should not exist considered abnormal if the individual has no symptoms associated with it. For example, Miguel Indurain, a Spanish cyclist and five time Tour de France winner, had a resting eye charge per unit of 28 beats per minute,[54] one of the everyman ever recorded in a salubrious homo. Daniel Green achieved the world record for the slowest heartbeat in a healthy human with a heart charge per unit of just 26 bpm in 2014.[55]
Arrhythmia [edit]
Arrhythmias are abnormalities of the heart rate and rhythm (sometimes felt as palpitations). They can be divided into 2 wide categories: fast and slow heart rates. Some cause few or minimal symptoms. Others produce more serious symptoms of lightheadedness, dizziness and fainting.[56]
Correlation with cardiovascular mortality hazard [edit]
A number of investigations indicate that faster resting eye rate has emerged as a new risk gene for bloodshed in homeothermic mammals, specially cardiovascular mortality in human beings. Faster heart rate may accompany increased product of inflammation molecules and increased production of reactive oxygen species in cardiovascular system, in improver to increased mechanical stress to the heart. There is a correlation between increased resting rate and cardiovascular take chances. This is not seen to exist "using an allotment of heart beats" but rather an increased risk to the system from the increased rate.[1]
An Australian-led international written report of patients with cardiovascular affliction has shown that heart beat rate is a key indicator for the take a chance of heart set on. The report, published in The Lancet (September 2008) studied 11,000 people, beyond 33 countries, who were existence treated for heart problems. Those patients whose heart charge per unit was above lxx beats per minute had significantly college incidence of heart attacks, hospital admissions and the need for surgery. Higher heart rate is idea to exist correlated with an increment in eye attack and about a 46 percent increase in hospitalizations for non-fatal or fatal middle assault.[57]
Other studies have shown that a high resting heart rate is associated with an increase in cardiovascular and all-cause mortality in the general population and in patients with chronic diseases.[58] [59] A faster resting heart charge per unit is associated with shorter life expectancy [1] [sixty] and is considered a strong take a chance cistron for heart affliction and eye failure,[61] independent of level of physical fitness.[62] Specifically, a resting heart rate higher up 65 beats per minute has been shown to have a stiff independent effect on premature bloodshed; every 10 beats per minute increase in resting heart rate has been shown to be associated with a x–20% increase in hazard of death.[63] In 1 study, men with no bear witness of heart disease and a resting heart rate of more than ninety beats per minute had a v times higher risk of sudden cardiac decease.[61] Similarly, another study found that men with resting middle rates of over 90 beats per minute had an well-nigh two-fold increase in chance for cardiovascular disease mortality; in women it was associated with a iii-fold increase.[60]
Given these data, heart rate should be considered in the assessment of cardiovascular chance, even in obviously good for you individuals.[64] Heart charge per unit has many advantages every bit a clinical parameter: It is cheap and quick to measure and is easily understandable.[65] Although the accepted limits of heart charge per unit are betwixt threescore and 100 beats per minute, this was based for convenience on the calibration of the squares on electrocardiogram paper; a better definition of normal sinus heart rate may be between 50 and 90 beats per minute.[66] [58]
Standard textbooks of physiology and medicine mention that eye rate (HR) is readily calculated from the ECG every bit follows: HR = g*sixty/RR interval in milliseconds, HR = lx/RR interval in seconds, or Hr = 300/number of big squares between successive R waves. In each example, the authors are actually referring to instantaneous HR, which is the number of times the heart would beat if successive RR intervals were constant.
Lifestyle and pharmacological regimens may be beneficial to those with loftier resting heart rates.[63] Exercise is one possible measure out to accept when an individual's heart rate is higher than lxxx beats per minute.[65] [67] Diet has also been constitute to be beneficial in lowering resting middle rate: In studies of resting heart rate and chance of death and cardiac complications on patients with type 2 diabetes, legumes were found to lower resting heart charge per unit.[68] This is idea to occur because in addition to the directly beneficial furnishings of legumes, they also displace animal proteins in the diet, which are college in saturated fat and cholesterol.[68] Another nutrient is omega-3 long chain polyunsaturated fatty acids (omega-3 fatty acid or LC-PUFA). In a meta-analysis with a full of 51 randomized controlled trials (RCTs) involvingy three,000 participants, the supplement mildly but significantly reduced middle rate (-2.23 bpm; 95% CI: -three.07, -i.forty bpm). When docosahexaenoic acrid (DHA) and eicosapentaenoic acid (EPA) were compared, small-scale heart rate reduction was observed in trials that supplemented with DHA (-two.47 bpm; 95% CI: -3.47, -1.46 bpm), but not in those received EPA.[69]
A very slow heart rate (bradycardia) may exist associated with heart cake.[70] It may besides arise from autonomous nervous system damage.[ medical citation needed ]
See also [edit]
- Heart rate monitor
- Cardiac cycle
- Electrocardiography
- Sinus rhythm
Notes [edit]
- ^ a b c Zhang GQ, Zhang W (2009). "Heart rate, lifespan, and mortality gamble". Ageing Inquiry Reviews. 8 (ane): 52–lx. doi:x.1016/j.arr.2008.ten.001. PMID 19022405. S2CID 23482241.
- ^ a b "All Nearly Heart Charge per unit (Pulse)". All About Centre Charge per unit (Pulse). American Centre Association. 22 Aug 2017. Retrieved 25 January 2018.
- ^ "Tachycardia| Fast Centre Rate". Tachycardia. American Heart Association. 2 May 2013. Retrieved 21 May 2014.
- ^ a b c Fuster, Wayne & O'Rouke 2001, pp. 78–79.
- ^ Schmidt-Nielsen, Knut (1997). Fauna physiology: accommodation and environment (5th ed.). Cambridge: Cambridge Univ. Press. p. 104. ISBN978-0-521-57098-5.
- ^ a b c Aladin, Amer I.; Whelton, Seamus P.; Al-Mallah, Mouaz H.; Blaha, Michael J.; Keteyian, Steven J.; Juraschek, Stephen P.; Rubin, Jonathan; Brawner, Clinton A.; Michos, Erin D. (2014-12-01). "Relation of resting heart rate to run a risk for all-crusade mortality by gender afterward because exercise capacity (the Henry Ford exercise testing project)". The American Journal of Cardiology. 114 (xi): 1701–06. doi:ten.1016/j.amjcard.2014.08.042. PMID 25439450.
- ^ a b c Hjalmarson, A.; Gilpin, E. A.; Kjekshus, J.; Schieman, G.; Nicod, P.; Henning, H.; Ross, J. (1990-03-01). "Influence of heart rate on bloodshed after astute myocardial infarction". The American Journal of Cardiology. 65 (9): 547–53. doi:10.1016/0002-9149(90)91029-half-dozen. PMID 1968702.
- ^ a b c Mason, Jay W.; Ramseth, Douglas J.; Chanter, Dennis O.; Moon, Thomas Due east.; Goodman, Daniel B.; Mendzelevski, Boaz (2007-07-01). "Electrocardiographic reference ranges derived from 79,743 ambulatory subjects". Journal of Electrocardiology. 40 (3): 228–34. doi:10.1016/j.jelectrocard.2006.09.003. PMID 17276451.
- ^ a b c Spodick, D. H. (1993-08-xv). "Survey of selected cardiologists for an operational definition of normal sinus centre rate". The American Journal of Cardiology. 72 (5): 487–88. doi:10.1016/0002-9149(93)91153-nine. PMID 8352202.
- ^ PubChem. "Atropine". pubchem.ncbi.nlm.nih.gov . Retrieved 2021-08-08 .
- ^ Richards, John R.; Garber, Dariush; Laurin, Erik G.; Albertson, Timothy E.; Derlet, Robert West.; Amsterdam, Ezra A.; Olson, Kent R.; Ramoska, Edward A.; Lange, Richard A. (June 2016). "Treatment of cocaine cardiovascular toxicity: a systematic review". Clinical Toxicology (Philadelphia, Pa.). 54 (5): 345–64. doi:10.3109/15563650.2016.1142090. ISSN 1556-9519. PMID 26919414. S2CID 5165666.
- ^ "All About Middle Rate (Pulse)". www.centre.org . Retrieved 2021-08-08 .
- ^ Anderson JM (1991). "Rehabilitating elderly cardiac patients". West. J. Med. 154 (5): 573–78. PMC1002834. PMID 1866953.
- ^ Hall, Arthur C. Guyton, John E. (2005). Textbook of medical physiology (11th ed.). Philadelphia: W.B. Saunders. pp. 116–22. ISBN978-0-7216-0240-0.
- ^ a b c d eastward f g h i j thousand fifty grand n o p q r south t u v westward Betts, J. Gordon (2013). Beefcake & physiology. pp. 787–846. ISBN978-1938168130 . Retrieved eleven August 2014.
- ^ Garcia A, Marquez MF, Fierro EF, Baez JJ, Rockbrand LP, Gomez-Flores J (May 2020). "Cardioinhibitory syncope: from pathophysiology to treatment-should nosotros think on cardioneuroablation?". J Interv Card Electrophysiol. 59 (2): 441–61. doi:10.1007/s10840-020-00758-2. PMID 32377918. S2CID 218527702.
- ^ Mustonen, Veera; Pantzar, Mika (2013). "Tracking social rhythms of the middle". Approaching Religion. 3 (2): sixteen–21. doi:10.30664/ar.67512.
- ^ Brosschot, J.F.; Thayer, J.F. (2003). "Middle rate response is longer subsequently negative emotions than subsequently positive emotions". International Journal of Psychophysiology. l (3): 181–87. doi:ten.1016/s0167-8760(03)00146-6. PMID 14585487.
- ^ Chou, C.Y.; Marca, R.Fifty.; Steptoe, A.; Brewin, C.R. (2014). "Heart rate, startle response, and intrusive trauma memories". Psychophysiology. 51 (three): 236–46. doi:10.1111/psyp.12176. PMC4283725. PMID 24397333.
- ^ Kim, Hye-Geum; Cheon, Eun-Jin; Bai, Dai-Seg; Lee, Immature Hwan; Koo, Bon-Hoon (March 2018). "Stress and Centre Rate Variability: A Meta-Assay and Review of the Literature". Psychiatry Investigation. xv (3): 235–45. doi:x.30773/pi.2017.08.17. ISSN 1738-3684. PMC5900369. PMID 29486547.
- ^ Fahlman, Andreas; Cozzi, Bruno; Manley, Mercy; Jabas, Sandra; Malik, Marek; Blawas, Ashley; Janik, Vincent 1000. (2020). "Conditioned Variation in Heart Rate During Static Breath-Holds in the Bottlenose Dolphin (Tursiops truncatus)". Frontiers in Physiology. 11: 604018. doi:10.3389/fphys.2020.604018. PMC7732665. PMID 33329056. S2CID 227128277. Lay summary.
- ^ Sherwood, L. (2008). Human being Physiology, From Cells to Systems. p. 327. ISBN9780495391845 . Retrieved 2013-03-10 .
- ^ MedlinePlus Encyclopedia: Pulse
- ^ Berne, Robert; Levy, Matthew; Koeppen, Bruce; Stanton, Bruce (2004). Physiology . Elsevier Mosby. p. 276. ISBN978-0-8243-0348-8.
- ^ "HRmax (Fettle)". MiMi.
- ^ Atwal S, Porter J, MacDonald P (February 2002). "Cardiovascular furnishings of strenuous practice in adult recreational hockey: the Hockey Center Written report". CMAJ. 166 (3): 303–07. PMC99308. PMID 11868637.
- ^ Chhabra, Lovely; Goel, Narender; Prajapat, Laxman; Spodick, David H; Goyal, Sanjeev (2012-01-31). "Mouse Heart Rate in a Human: Diagnostic Mystery of an Extreme Tachyarrhythmia". Indian Pacing and Electrophysiology Journal. 12 (1): 32–35. doi:10.1016/s0972-6292(sixteen)30463-6. PMC3273956. PMID 22368381.
- ^ Froelicher, Victor; Myers, Jonathan (2006). Exercise and the Centre (5th ed.). Philadelphia: Elsevier. pp. 9, 108–12. ISBN978-1-4160-0311-three.
- ^ a b Nes, B.M.; Janszky, I.; Wisloff, U.; Stoylen, A.; Karlsen, T. (December 2013). "Age‐predicted maximal heart rate in healthy subjects: The Hunt Fitness Study". Scandinavian Journal of Medicine & Science in Sports. 23 (6): 697–704. doi:10.1111/j.1600-0838.2012.01445.x. PMID 22376273. S2CID 2380139.
- ^ a b Tanaka H, Monahan KD, Seals DR (Jan 2001). "Age-predicted maximal heart charge per unit revisited". J. Am. Coll. Cardiol. 37 (one): 153–56. doi:10.1016/S0735-1097(00)01054-8. PMID 11153730.
- ^ Gellish, Ronald L.; Goslin, Brian R.; Olson, Ronald E.; McDONALD, Audry; Russi, Gary D.; Moudgil, Virinder K. (May 2007). "Longitudinal Modeling of the Relationship between Age and Maximal Heart Charge per unit". Medicine & Scientific discipline in Sports & Do. 39 (5): 822–829. doi:10.1097/mss.0b013e31803349c6. PMID 17468581.
- ^ "Target Heart Rate and Estimated Maximum Eye Rate". U.S. Centers for Disease Control and Prevention (CDC). 14 October 2020. Retrieved 16 November 2021.
{{cite web}}: CS1 maint: url-status (link) - ^ a b c d e f k h Kolata, Gina (2001-04-24). "'Maximum' Heart Rate Theory Is Challenged". New York Times.
- ^ a b c Robergs R, Landwehr R (2002). "The Surprising History of the 'HRmax=220-age' Equation". Journal of Exercise Physiology. 5 (2): 1–ten. CiteSeerXten.1.1.526.6164.
- ^ Inbar O., Oten A., Scheinowitz M., Rotstein A., Dlin R., Casaburi R. (1994). "Normal cardiopulmonary responses during incremental practise in 20-seventy-yr-old men". Med Sci Sports Exerc. 26 (5): 538–546. doi:10.1249/00005768-199405000-00003. PMID 8007799.
{{cite periodical}}: CS1 maint: multiple names: authors listing (link) - ^ Gulati M, Shaw LJ, Thisted RA, Black Hr, Bairey Merz CN, Arnsdorf MF (2010). "Eye rate response to exercise stress testing in asymptomatic women: the st. James women take center project". Circulation. 122 (2): 130–37. doi:10.1161/CIRCULATIONAHA.110.939249. PMID 20585008.
- ^ Wohlfart B, Farazdaghi GR (May 2003). "Reference values for the physical piece of work capacity on a bicycle ergometer for men -- a comparison with a previous written report on women". Clin Physiol Funct Imaging. 23 (iii): 166–70. doi:10.1046/j.1475-097X.2003.00491.x. PMID 12752560. S2CID 25560062.
- ^ Farazdaghi GR, Wohlfart B (November 2001). "Reference values for the concrete work capacity on a bicycle ergometer for women between 20 and lxxx years of age". Clin Physiol. 21 (6): 682–87. doi:10.1046/j.1365-2281.2001.00373.x. PMID 11722475.
- ^ Lounana J, Campion F, Noakes TD, Medelli J (2007). "Human relationship between %HRmax, %HR reserve, %VO2max, and %VO2 reserve in elite cyclists". Med Sci Sports Exerc. 39 (2): 350–57. doi:10.1249/01.mss.0000246996.63976.5f. PMID 17277600.
- ^ Karvonen MJ, Kentala Eastward, Mustala O (1957). "The effects of grooming on heart rate; a longitudinal study". Ann Med Exp Biol Fenn. 35 (3): 307–15. PMID 13470504.
- ^ Boyfriend DP, Leutholtz BC, King ME, Haas LA, Branch JD (1998). "Relationship between % heart rate reserve and % VO2 reserve in treadmill exercise". Med Sci Sports Exerc. 30 (2): 318–21. doi:10.1097/00005768-199802000-00022. PMID 9502363.
- ^ Karvonen J, Vuorimaa T (May 1988). "Eye rate and practice intensity during sports activities. Practical application". Sports Medicine. v (5): 303–11. doi:x.2165/00007256-198805050-00002. PMID 3387734. S2CID 42982362.
- ^ Zoladz, Jerzy A. (2018). Muscle and Do Physiology (beginning ed.). Elsevier. ISBN9780128145937.
- ^ a b Cole CR, Blackstone EH, Pashkow FJ, Snader CE, Lauer MS (1999). "Eye-rate recovery immediately afterwards exercise every bit a predictor of mortality". Northward Engl J Med. 341 (xviii): 1351–57. doi:x.1056/NEJM199910283411804. PMID 10536127.
- ^ a b c d eastward Froelicher, Victor; Myers, Jonathan (2006). Exercise and the Heart (fifth ed.). Philadelphia: Elsevier. p. 114. ISBN978-1-4160-0311-3.
- ^ Emren, SV; Gediz, RB; Şenöz, O; Karagöz, U; Şimşek, EÇ; Levent, F; Özdemir, E; Gürsoy, MO; Nazli, C (February 2019). "Decreased middle charge per unit recovery may predict a loftier SYNTAX score in patients with stable coronary artery affliction". Bosnian Journal of Basic Medical Sciences. 19 (1): 109–15. doi:10.17305/bjbms.2019.3725. PMC6387669. PMID 30599115.
- ^ "Homo Heart Trivia". The Franklin Found. 2015-06-02. Retrieved 2021-08-08 .
- ^ "Embryonic Heart Rates Compared in Assisted and Non-Assisted Pregnancies". Contemporary OB/GYN.
- ^ Fuster, Wayne & O'Rouke 2001, pp. 824–29.
- ^ Regulation of Human Centre Rate Archived 2007-05-xiv at the Wayback Machine. Serendip. Retrieved on June 27, 2007.
- ^ Salerno DM, Zanetti J (1991). "Seismocardiography for monitoring changes in left ventricular function during ischemia". Breast. 100 (4): 991–93. doi:10.1378/chest.100.iv.991. PMID 1914618. S2CID 40190244.
- ^ Puyo, Léo; Paques, Michel; Fink, Mathias; Sahel, José-Alain; Atlan, Michael (2019-09-05). "Waveform assay of human retinal and choroidal blood flow with laser Doppler holography". Biomedical Optics Limited. x (ten): 4942–4963. arXiv:2106.00634. doi:ten.1364/BOE.10.004942. PMC6788604. PMID 31646021.
- ^ "Bradycardia - Symptoms and causes". Mayo Clinic . Retrieved 2021-08-08 .
- ^ Guinness Earth Records 2004 (Bantam ed.). New York: Bantam Books. 2004. pp. 10–eleven. ISBN978-0-553-58712-8.
- ^ "Slowest centre rate: Daniel Dark-green breaks Guinness Globe Records record". World Record Academy. 29 November 2014.
- ^ "Eye arrhythmia - Symptoms and causes". Mayo Dispensary . Retrieved 2021-08-08 .
- ^ Fox K, Ford I (2008). "Centre rate as a prognostic gamble factor in patients with coronary artery illness and left-ventricular systolic dysfunction (BEAUTIFUL): a subgroup assay of a randomised controlled trial". Lancet. 372 (half dozen): 817–21. doi:x.1016/S0140-6736(08)61171-X. PMID 18757091. S2CID 6481363.
- ^ a b Jiang 10, Liu X, Wu South, Zhang GQ, Peng Chiliad, Wu Y, Zheng X, Ruan C, Zhang W (Jan 2015). "Metabolic syndrome is associated with and predicted by resting heart rate: a cross-sectional and longitudinal study". Eye. 101 (one): 44–9. doi:10.1136/heartjnl-2014-305685. PMID 25179964.
- ^ Cook, Stéphane; Hess, Otto 1000. (2010-03-01). "Resting heart rate and cardiovascular events: time for a new crusade?". European Centre Journal. 31 (5): 517–19. doi:ten.1093/eurheartj/ehp484. PMID 19933283.
- ^ a b Cooney, Marie Therese; Vartiainen, Erkki; Laatikainen, Tiina; Laakitainen, Tinna; Juolevi, Anne; Dudina, Alexandra; Graham, Ian Thousand. (2010-04-01). "Elevated resting heart rate is an independent take a chance factor for cardiovascular disease in healthy men and women". American Centre Journal. 159 (4): 612–19.e3. doi:10.1016/j.ahj.2009.12.029. PMID 20362720.
- ^ a b Teodorescu, Carmen; Reinier, Kyndaron; Uy-Evanado, Audrey; Gunson, Karen; Jui, Jonathan; Chugh, Sumeet South. (2013-08-01). "Resting heart charge per unit and risk of sudden cardiac expiry in the general population: influence of left ventricular systolic dysfunction and eye rate-modulating drugs". Eye Rhythm. 10 (viii): 1153–58. doi:10.1016/j.hrthm.2013.05.009. PMC3765077. PMID 23680897.
- ^ Jensen, Magnus Thorsten; Suadicani, Poul; Hein, Hans Ole; Gyntelberg, Finn (2013-06-01). "Elevated resting eye charge per unit, physical fitness and all-cause mortality: a xvi-twelvemonth follow-upward in the Copenhagen Male Study". Heart. 99 (12): 882–87. doi:10.1136/heartjnl-2012-303375. PMC3664385. PMID 23595657.
- ^ a b Woodward, Mark; Webster, Ruth; Murakami, Yoshitaka; Barzi, Federica; Lam, Tai-Hing; Fang, Xianghua; Suh, Il; Batty, G. David; Huxley, Rachel (2014-06-01). "The association between resting heart charge per unit, cardiovascular disease and mortality: evidence from 112,680 men and women in 12 cohorts". European Journal of Preventive Cardiology. 21 (6): 719–26. doi:ten.1177/2047487312452501. PMID 22718796. S2CID 31791634.
- ^ Arnold, J. Malcolm; Fitchett, David H.; Howlett, Jonathan G.; Lonn, Eva K.; Tardif, Jean-Claude (2008-05-01). "Resting eye charge per unit: a modifiable prognostic indicator of cardiovascular take chances and outcomes?". The Canadian Periodical of Cardiology. 24 Suppl A: 3A–8A. doi:10.1016/s0828-282x(08)71019-5. PMC2787005. PMID 18437251.
- ^ a b Nauman, Javaid (2012-06-12). "Why mensurate resting heart rate?". Tidsskrift for den Norske Lægeforening. 132 (11): 1314. doi:10.4045/tidsskr.12.0553. PMID 22717845.
- ^ Spodick, DH (1992). "Operational definition of normal sinus eye rate". Am J Cardiol. 69 (14): 1245–46. doi:10.1016/0002-9149(92)90947-West. PMID 1575201.
- ^ Sloan, Richard P.; Shapiro, Peter A.; DeMeersman, Ronald Due east.; Bagiella, Emilia; Brondolo, Elizabeth Northward.; McKinley, Paula Due south.; Slavov, Iordan; Fang, Yixin; Myers, Michael M. (2009-05-01). "The effect of aerobic grooming and cardiac autonomic regulation in young adults". American Periodical of Public Wellness. 99 (5): 921–28. doi:ten.2105/AJPH.2007.133165. PMC2667843. PMID 19299682.
- ^ a b Jenkins, David J. A.; Kendall, Cyril W. C.; Augustin, Livia S. A.; Mitchell, Sandra; Sahye-Pudaruth, Sandhya; Blanco Mejia, Sonia; Chiavaroli, Laura; Mirrahimi, Arash; Ireland, Christopher (2012-11-26). "Effect of legumes as office of a low glycemic alphabetize diet on glycemic control and cardiovascular risk factors in blazon two diabetes mellitus: a randomized controlled trial". Archives of Internal Medicine. 172 (21): 1653–60. doi:10.1001/2013.jamainternmed.seventy. PMID 23089999.
- ^ Hidayat Grand, Yang J, Zhang Z, Chen GC, Qin LQ, Eggersdorfer Yard, Zhang W (Jun 2018). "Effect of omega-iii long-chain polyunsaturated fatty acrid supplementation on heart rate: a meta-analysis of randomized controlled trials". European Journal of Clinical Nutrition. 72 (6): 805–817. doi:10.1038/s41430-017-0052-3. PMC5988646. PMID 29284786.
- ^ Atrioventricular Block at eMedicine
References [edit]
- This commodity incorporates text from the CC-Past book: OpenStax College, Beefcake & Physiology. OpenStax CNX. 30 Jul 2014.
Bibliography [edit]
- Fuster, Valentin; Wayne, Alexander R.; O'Rouke, Robert A. (2001). Hurst'southward The Centre (10th International ed.). New York: McGraw-Colina. ISBN978-0071162968. OCLC 49034333.
- Jarvis, C. (2011). Physical Test and Health Assessment (six ed.). Saunders Elsevier. ISBN978-1437701517.
External links [edit]
- Online Heart Beats Per Infinitesimal Reckoner Tap along with your heart rate
- An application (open-source) for contactless real time eye charge per unit measurements by means of an ordinary web cam
Source: https://en.wikipedia.org/wiki/Heart_rate


0 Response to "What Is the Heart Rate for a Baby at 7 Weeks and 6 Days"
Enregistrer un commentaire